New Imaging Data Tells Story of Travelling Tau
Quick Links
As more scientists delve into the possibilities offered by imaging the second major protein pathology of Alzheimer’s disease, aggregates of tau, they are getting a close-up, live view of how this pathology relates to neurodegeneration and cognitive decline. At the Alzheimer's Association International Conference 2015, held July 18 to 23 in Washington, D.C., tau imaging data bolstered the idea that tau sits tight in the medial temporal lobe until Aβ builds up, then it spreads, wreaking havoc on cognition. New imaging data suggests that once it breaks loose, tau spreads through functional networks and impairs brain metabolism. What’s more, unlike Aβ, which appears diffusely throughout the brain, tau deposits seem to map closely onto regions where atrophy occurs and cognitive deficits originate. “Unlike amyloid imaging, tau PET seems to strongly correlate with cognition and clinical states,” said Gil Rabinovici, University of California, San Francisco. Researchers were also excited by a new tau ligand that appears to have better specificity and kinetics than its predecessors.
Roche Forges Ahead with New Tracer
Scientists collaborating with F. Hoffmann-La Roche in Basel, Switzerland, introduced the first human data on an up-and-coming tau PET ligand, [18F]RO6958948. Dean Wong and Hiroto Kuwabara from Johns Hopkins University in Baltimore presented two posters detailing preliminary data from a Phase 1 trial of this ligand and two others, [11C]RO6924963 and [11C]RO6931643. So far they have scanned seven young, healthy controls aged 25 to 38, and seven people with mild to moderate Alzheimer’s disease aged 64 to 86. Each person was scanned twice, one to two weeks apart, with two different tracers, so that the researchers could directly compare ligands.
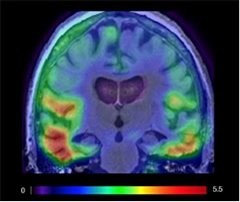
Roche’s Lead Tau Tracer:
Ro6958948 binds areas expected to contain tau in a patient with AD. [Courtesy of Roche.]
Ro6931643 and Ro6958948 cleared quickly from controls and clearly differentiated them from AD patients, said Wong. These two tracers bound to frontal, temporal, parietal, and occipital cortices, fusiform and hippocampal gyri, and the entorhinal area in patients (see image at right). This pattern resembles that seen in Braak stage V/VI (Braak and Braak, 1991). Controls had weak but visible uptake in the dorsal cerebellum, which has been reported with other tau tracers. Subjects’ brains took up moderate amounts of Ro6931643, with a standard uptake value (SUV) of about 1.5 between 60 and 90 minutes. Ro6958948 entered the brain more readily, reaching an SUV of up to 3.5 the same time frame. Of the three compounds, Ro6924963 proved most problematic. It failed to enter the brain well, then stuck around in controls when it should have washed out quickly, Wong said.
Roche is now moving forward with Ro6958948. Scientists are examining its test-retest reliability by scanning five additional AD patients and five age-matched controls, two weeks apart, to see how binding varies. They will also scan out to 200 minutes to better determine tracer kinetics, and choose the best reference region—likely the pons or cerebellum.
How does Ro6958948 compare with other tau tracers in development? A head-to-head comparison has yet to be done, said Roche’s Edilio Borroni. Ro6958948 appears to have a better kinetic profile than one of the leading tau tracers, T807/AV1451, Borroni said. Binding of T807/AV1451 never stabilizes in the cortex during the scanning period. The tracer also has different kinetics in different brain regions (Feb 2015 news). By contrast, Ro6958948 uptake stabilizes quickly, and at relatively uniform times for all brain regions. These qualities could make it easier in longitudinal studies to detect subtle changes in tau load, said Robert Comley, also from Roche. In addition, researchers see fewer artifacts with Ro6958948. It does not label the choroid plexus, as does T807/AV1451, and the striatum takes up less Ro6958948 than it does THK5351 or T807/AV1451, said Comley.
Though more data are needed, these qualities may give Ro6958948 a competitive edge, said researchers at the conference. “This tracer is an interesting and promising one,” said Keith Johnson, Massachusetts General Hospital, Boston. “There’s been an evolution, a continuous improvement with amyloid tracers, and hopefully we’ll see that with tau, too,” he said.
“The work that they’ve done looks careful and thorough,” said Chet Mathis, University of Pittsburgh, who agreed that the early data make Ro6958948 look promising. It demonstrates a good tissue-to-plasma ratio and fast kinetics, he said, and the background washes out quickly in controls. He noted that the compound binds in places that contain no tau, but this off-target binding falls below that seen in THK5351 or T807/AV1451. This off-target binding is a common issue for tau tracers, said Bill Jagust, University of California, Berkeley. Figuring out what they are binding may help explain something about tau, he said.
Amyloid Triggers Tau Spread and Destruction
At AAIC, more evidence emerged to support the notion that Aβ accumulation causes tau to spread from the medial temporal lobe and wreak havoc (Feb 2015 news).
Michael Schöll, who works with Jagust, correlated T807/AV1451 uptake with cognition among 27 normal people, average age 79, from the Berkeley Aging Cohort Study. He found that ligand binding in the entorhinal cortex and hippocampus correlated with slightly poorer and deteriorating episodic memory. This fits with the primary age-related tauopathy (PART) reported almost universally in elderly people (Crary et al., 2014). However, in those who were also amyloid-positive, surrounding areas, such as the inferior and lateral temporal cortex, as well as lateral and medial frontal and parietal cortex, took up the tracer too, and the global cognitive score started to decline. “It’s seems that once you have amyloid, tau moves outside the medial temporal lobe and global cognition is affected,” Schöll told Alzforum. He cautioned that the results cannot say whether the tau spread or amyloid comes first, and noted that the small sample size and some uncertainties about what PET tracers bind limit the conclusions he can draw. “Now the questions are how this tau pattern develops, and what is making it spread into these particular regions,” said Jagust.
If tau does compromise cognition, could that manifest in other ways? Bernard Hanseeuw, from Johnson’s lab, tested if tau or amyloid deposition brought about hypometabolism in the parietal cortex, which occurs early in Alzheimer’s disease (Herholz 2010). Hanseeuw and colleagues performed PET using PiB, T807/AV1451, and FDG on 90 cognitively normal people, averaging age 74, from the Harvard Aging Brain Study. They found that tau accumulation in the entorhinal cortex associated with reduced metabolism in the parietal, regardless of amyloid. However, metabolism dropped even lower if amyloid had built up and tau had spread into the inferior temporal cortex. Hanseeuw said the results suggest that tau tangles in the entorhinal cortex cause some hypometabolism during normal aging. However, in Alzheimer’s disease, when amyloid accumulates and causes tau to spread into the inferior temporal cortex, the problem worsens. It also hints that the entorhinal and parietal cortices are functionally linked, and that tau affects that connection, he said. The group next plans to look at additional regions of hypometabolism, he told Alzforum.
Victor Villemagne of the University of Melbourne, Australia, commented that the findings could explain suspected non-amyloid pathology, or SNAP, which is defined by a negative Aβ biomarker in the presence of a marker of neurodegeneration, such as hypometabolism on an FDG-PET scan.
Disaster Strikes Wherever Tau Lands
Once outside the medial temporal lobe, tau seems to cause trouble wherever it lands. At AAIC, Daniel Schonhaut, who works with Rabinovici, expanded on the notion that tau builds up in brain regions thought to underlie clinical symptoms in patients with atypical forms of AD (Feb 2015 conference news). He compared performance on a variety of cognitive tests with T807/AV1451 scans from 19 patients with typical and atypical forms of AD, including posterior cortical atrophy, primary progressive aphasia, and corticobasal syndrome.
Schonhaut reported that AD patients who performed more poorly on memory tasks had more tau in the hippocampus and surrounding medial temporal areas, while patients with visuospatial deficits had more tau in occipital regions (see image below). Those with language difficulties, meanwhile, had more tau in left temporoparietal regions associated with language function. “The distribution patterns of tau we’re seeing with this PET tracer seem to underlie the clinical phenotype of our patients,” Schonhaut told Alzforum
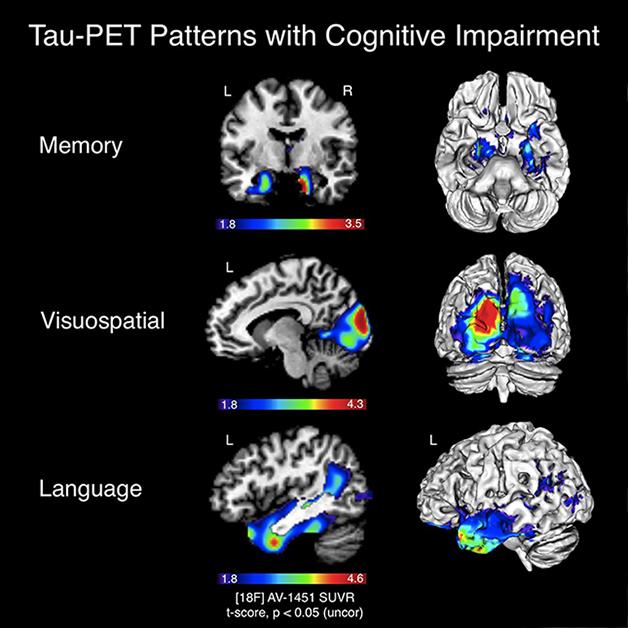
Close Match: Areas of T807/AV1451 uptake align with regions associated with cognitive deficits. [Courtesy of the Rabinovici lab.]
“These data show nicely that there’s a relationship between where the tau is clinical symptomatology,” said Jagust. “We haven’t seen that with amyloid.” Rabinovici noted that these results corroborate findings from classic postmortem studies demonstrating that cognitive state correlates much more strongly with tangle than amyloid pathology. They also support tau as a therapeutic target, particularly in the symptomatic phase of AD, he told Alzforum.
Researchers are also finding that tau deposition aligns with areas of cortical thinning. Chenjie Xia, who works with Brad Dickerson at Massachusetts General Hospital in Boston, analyzed T807/AV1451 scans and structural MRI images of five patients, two with amnestic AD, and one each with posterior cortical atrophy, primary progressive aphasia, and corticobasal syndrome. In each case, the T807/AV1451 signal correlated with areas that atrophied the most. Those areas also corresponded with the expected areas of atrophy for each disease. For instance, the two patients with amnestic AD took up tracer in the bilateral parietal and medial temporal areas, which lost volume compared with those areas in controls. In the PCA patient with visual deficits, the tracer labeled atrophied occipital regions. In the PPA patient, T807/AV1451 bound in the left parietal lobe, and in the person with CBS, in the primary and association sensorimotor cortices, each time matching the pattern of cortical thinning. In all cases, the tau deposition correlated significantly with the areas of atrophy, but amyloid did not, Xia said.
How Does Tau Spread?
Though these results all point to tau’s destructive nature, none gives clues as to how tau is transported through the brain. The idea that it travels trans-synaptically has gained traction. Evidence from cell culture and animal models suggest as much, but scientists still question whether it spreads this way in humans (Mar 2013 conference news; Apr 2015 conference news). At AAIC, Joseph Seemiller, working with Alexander Drzezga, University of Cologne, Germany, claimed it does. They used imaging to correlate patterns of tau distribution with known connectivity maps of the brain.
By comparing T807/AV1451 images, the researchers subtracted the “normal” signal of 18 healthy controls from those of 18 AD patients to identify AD-specific regions of tauopathy. From these they found one spot, near the angular gyrus, where tau aggregated the most. Voxels closest and most functionally connected to this “tau max” accumulated more of the misfolded protein. This supports the idea that tau spreads outward from an epicenter and along functional networks, Seemiller told Alzforum.
To find out if that is the case, they compared the pattern of T807/AV1451 uptake to 14 known functional networks, including those for language, visuospatial, and auditory functioning. The posterior default mode network (DMN) strongly matched the pattern of ligand distribution. The precuneus, language, and higher visual networks correlated, too. The DMN is a site of early Aβ deposition in AD and activity there wanes early in disease, leading some to suggest the network may be particularly vulnerable to pathology (Feb 2009 news; Mar 2004 news).
Michael Greicius, Stanford University, California, told Alzforum that the findings suggest that tau spreads between functionally connected synapses in the human brain. “The idea that tau spreads through interconnected networks is appealing,” said Rabinovici. However, both scientists said more research is needed to prove it. It is unclear why tau would spread along predefined functional networks, said Seemiller. He said that direct evidence can only come from experiments at the molecular level.—Gwyneth Dickey Zakaib
References
News Citations
- Mixed Bag on Tau Tracer Validation, Kinetics: Some Things Fit, Some Don’t
- Tau Tracer T807/AV1451 Tracks Neurodegenerative Progression
- What If It’s Not Garden-Variety AD? Telling Variants Apart by Where Tau Is
- Tau, α-Synuclein Spread: Crazy Stuff—How Might It Work?
- Protein Propagation Real, but Mechanisms Hazy
- Cortical Hubs Found Capped With Amyloid
- Network Diagnostics: "Default-Mode" Brain Areas Identify Early AD
Paper Citations
- Braak H, Braak E. Neuropathological stageing of Alzheimer-related changes. Acta Neuropathol. 1991;82(4):239-59. PubMed.
- Crary JF, Trojanowski JQ, Schneider JA, Abisambra JF, Abner EL, Alafuzoff I, Arnold SE, Attems J, Beach TG, Bigio EH, Cairns NJ, Dickson DW, Gearing M, Grinberg LT, Hof PR, Hyman BT, Jellinger K, Jicha GA, Kovacs GG, Knopman DS, Kofler J, Kukull WA, Mackenzie IR, Masliah E, McKee A, Montine TJ, Murray ME, Neltner JH, Santa-Maria I, Seeley WW, Serrano-Pozo A, Shelanski ML, Stein T, Takao M, Thal DR, Toledo JB, Troncoso JC, Vonsattel JP, White CL 3rd, Wisniewski T, Woltjer RL, Yamada M, Nelson PT. Primary age-related tauopathy (PART): a common pathology associated with human aging. Acta Neuropathol. 2014 Dec;128(6):755-66. Epub 2014 Oct 28 PubMed.
- Herholz K. Cerebral glucose metabolism in preclinical and prodromal Alzheimer's disease. Expert Rev Neurother. 2010 Nov;10(11):1667-73. PubMed.
External Citations
Further Reading
Papers
- Cook CN, Murray ME, Petrucelli L. Understanding biomarkers of neurodegeneration: Novel approaches to detecting tau pathology. Nat Med. 2015 Mar;21(3):219-20. PubMed.
- James OG, Doraiswamy PM, Borges-Neto S. PET Imaging of Tau Pathology in Alzheimer's Disease and Tauopathies. Front Neurol. 2015;6:38. Epub 2015 Mar 9 PubMed.
- Ariza M, Kolb HC, Moechars D, Rombouts F, Andrés JI. Tau Positron Emission Tomography (PET) Imaging: Past, Present, and Future. J Med Chem. 2015 Jun 11;58(11):4365-82. Epub 2015 Feb 25 PubMed.
- Villemagne VL, Fodero-Tavoletti MT, Masters CL, Rowe CC. Tau imaging: early progress and future directions. Lancet Neurol. 2015 Jan;14(1):114-24. PubMed.
Annotate
To make an annotation you must Login or Register.

Comments
KULeuven
The reported work is encouraging but I, for one, propose a caveat: please separate tauopathy and protein tau in terms of spreading. While it has been clear for a long time that tauopathy is spreading from early- to later-affected brain regions, this does not imply that protein tau itself, in whatever physical form(s), is also spreading. One wonders what is really meant by "trans-synaptically." The direction of spreading is evidently afferent, i.e. toward the projection area, implying transfer from the pre- to the post-synaptic compartment at the synapse. Looking at images of synapses, one observes intense exo- and endocytic activity in and at the pre-synaptic membrane, but none at the post-synaptic side. In addition, one must remember that tau is a non-structured or naturally unfolded protein, with an overall length of about 130 to 160 nm (pending the splice-form); this corresponds to about 5-8 times the width of any synaptic cleft. Finally, to explain that tau-immunotherapy actually works most likely by trapping protein tau extracellularly to direct it for disposal (by any means), one must assume that antibodies engage inside the synaptic cleft to stop "trans-synaptic spreading".
Make a Comment
To make a comment you must login or register.