APP Sorting Protein May Link Alzheimer’s and Diabetes
Quick Links
Two pernicious disorders of late life, Alzheimer disease and diabetes, may be tied together by a common connection with a pathway that sorts and trafficks proteins such as APP within cells, new research suggests. In the September 29 issue of the Journal of Neuroscience, researchers led by Sam Gandy at Mount Sinai School of Medicine in New York City report that the sorting protein SorCS1 reduces Aβ generation when overexpressed, and conversely is associated with higher levels of Aβ in female mice when underexpressed. SorCS1 has been genetically linked to both diabetes and AD. The convergence of these two diseases on SorCS1 may help explain why having diabetes is a risk factor for contracting Alzheimer’s. The results also suggest a potential new pathway for therapeutic intervention into both disorders.
This paper is important, said Thomas Willnow of the Max-Delbrueck-Center for Molecular Medicine in Berlin, Germany, as it adds pieces to help solve the puzzle of the intracellular trafficking of APP. The data also fit well with previous reports finding that trafficking pathways may be altered in AD, Willnow said. “I think it all adds up and points to a very important aspect of [AD] pathology.”
When transmembrane proteins such as APP are endocytosed back into the cell, they can be directed to lysosomes for degradation, or back to the trans-Golgi network for recycling under the direction of a protein complex called the retromer. The retromer pathway of protein sorting was first described in mammals only six years ago, but evidence is mounting that it may play a role in the pathogenesis of AD. In flies and mice, retromer deficiency is associated with elevations of Aβ, as well as memory and synaptic defects, although the mechanism is unknown (see ARF related news story on Muhammad et al., 2008). Additionally, work led by Scott Small at Columbia University in New York City showed that retromer proteins Vps35 and Vps26 are reduced in the regions of AD brains most affected by the disease (see Small et al., 2005.)
Retromer proteins have been found to interact with a member of the sortilin family of sorting proteins, SorL1. SorL1 has been genetically linked to AD (see ARF related news story on Rogaeva et al., 2007), and currently occupies rank 7 in the AlzGene Top Results. In addition, SorL1 expression is reduced in cases of sporadic AD (see Dodson et al., 2006). SorL1 directly binds to APP and has been shown to affect Aβ processing (see ARF related news story on Schmidt et al., 2007). A related sortilin, SorCS1, is genetically linked not only to AD (see Liang et al., 2009), but also to Type I and II diabetes (see Goodarzi et al., 2007 ).
Gandy and colleagues wanted to find out if SorCS1, like SorL1, had a functional role in AD. To directly test the sorting protein’s effect on APP metabolism, first author Rachel Lane overexpressed both APP and the major brain transcript of SorCS1 in cell cultures. In cells with SorCS1, the C-terminal cleavage fragments of APP were reduced by about half compared to cells overexpressing only APP, and secreted Aβ was reduced by about one-third. Lane and colleagues then looked in vivo, this time at loss of SorCS1 function. In hypomorphic mice that expressed about half the normal level of SorCS1, the levels of C-terminal APP fragments went up by about one-quarter. In the female hypomorphs only, the level of Aβ increased significantly over wild-type levels. This gender difference is seen also in the genetic linkage studies, where SorCS1 is primarily a risk factor for women in both AD and diabetes, although the reason for this is unknown.
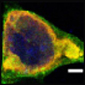
In transfected HEK293t cells, SorCS1 (red) co-localizes with APP (green) around the nucleus (blue). Image credit: Rachel Lane
The authors used co-immunoprecipitation to show that SorCS1 directly interacts with APP, SorL1, and Vps35, strengthening the idea that these proteins act in a complex. Furthermore, in the female SorCS1 hypomorphs, the levels of SorL1 and Vps35 were down. This might be due to coordinate transcriptional regulation of the complex, Gandy speculated, adding that this is something they plan to investigate.
The results highlight the importance of the retromer complex in APP metabolism, Gandy said. “Now we have two independent molecules, SorL1 and SorCS1, converging on the retromer as potentially being very important in the etiology of AD.” Small, a co-author on this paper, points out that multiple lines of evidence now implicate the retromer in AD pathology: not only data from cell culture and animal model experiments, but also genetic links between sorting proteins and AD, and the reduced levels of many retromer and sorting proteins in AD brains.
To follow up on these results, Gandy said they want to further characterize the SorCS1 hypomorphs in terms of learning, memory, and behavior, to get a better idea of what processes SorCS1 affects. Once they know that, Gandy said, they will cross these mice with AD mice that overexpress human APP, to get a more robust AD pathology and see how that is altered by loss of SorCS1 activity.
Small, meanwhile, is interested in the question of what the retromer pathway does in neurons. It is present in all cells, but the proteins are particularly highly expressed in brain. Do the specialized properties of neurons require retromers to act in specific ways in brain, for example to mediate long-range transport up and down processes, Small wonders? Using primary cultures of hippocampal neurons, Small plans to examine in what cellular compartment retromers act—in axons, in dendrites, at the pre-synapse or post-synapse? The answers, Small said, will help to inform scientists of how retromer dysfunction contributes to AD.
One of the most intriguing implications of the SorCS1 findings, Willnow said, is that SorCS1 might be a mechanistic link between AD and type II diabetes, helping to explain why diabetes is a risk factor for Alzheimer’s. “It opens up a completely new field,” Willnow said.
Gandy agrees. “We’re very excited, because SorCS1 gives a new target both for both diseases. We could ideally try to find a way to elevate the levels of these components and maybe have a compound that would work in the periphery to help with insulin sensitivity, and in the brain to help with AD.” However, Greg Cole at the University of California in Los Angeles cautioned in an email to ARF that “therapeutic relevance may be limited by issues of specificity with the more basic downstream sorting machinery,” since the sorting machinery is present in all cell types (see full comment below).
The protein sorting pathway may help to explain what happens in late-onset AD, where there are no mutations in APP or presenilin to account for the piling up of Aβ. “Over a lifetime, small differences in sorting rates from [genetic] variants that modestly impact Aß production rates may have dramatic long term impact,” Cole wrote. Small agrees, speculating that in sporadic AD, “Maybe you don’t need primary defects in the [APP] molecules themselves. Perhaps it’s enough to have defects in how you handle, sort, and traffic those molecules.”—Madolyn Bowman Rogers
References
News Citations
- Mice, Flies Further Implicate Retromer in AD Pathogenesis
- SORLA Soars—Large Study Links Gene to Late-onset AD
- Sorting Out SorLA—What Role in APP Processing, AD?
Paper Citations
- Muhammad A, Flores I, Zhang H, Yu R, Staniszewski A, Planel E, Herman M, Ho L, Kreber R, Honig LS, Ganetzky B, Duff K, Arancio O, Small SA. Retromer deficiency observed in Alzheimer's disease causes hippocampal dysfunction, neurodegeneration, and Abeta accumulation. Proc Natl Acad Sci U S A. 2008 May 20;105(20):7327-32. PubMed.
- Small SA, Kent K, Pierce A, Leung C, Kang MS, Okada H, Honig L, Vonsattel JP, Kim TW. Model-guided microarray implicates the retromer complex in Alzheimer's disease. Ann Neurol. 2005 Dec;58(6):909-19. PubMed.
- Rogaeva E, Meng Y, Lee JH, Gu Y, Kawarai T, Zou F, Katayama T, Baldwin CT, Cheng R, Hasegawa H, Chen F, Shibata N, Lunetta KL, Pardossi-Piquard R, Bohm C, Wakutani Y, Cupples LA, Cuenco KT, Green RC, Pinessi L, Rainero I, Sorbi S, Bruni A, Duara R, Friedland RP, Inzelberg R, Hampe W, Bujo H, Song YQ, Andersen OM, Willnow TE, Graff-Radford N, Petersen RC, Dickson D, Der SD, Fraser PE, Schmitt-Ulms G, Younkin S, Mayeux R, Farrer LA, St George-Hyslop P. The neuronal sortilin-related receptor SORL1 is genetically associated with Alzheimer disease. Nat Genet. 2007 Feb;39(2):168-77. PubMed.
- Dodson SE, Gearing M, Lippa CF, Montine TJ, Levey AI, Lah JJ. LR11/SorLA expression is reduced in sporadic Alzheimer disease but not in familial Alzheimer disease. J Neuropathol Exp Neurol. 2006 Sep;65(9):866-72. PubMed.
- Schmidt V, Sporbert A, Rohe M, Reimer T, Rehm A, Andersen OM, Willnow TE. SorLA/LR11 regulates processing of amyloid precursor protein via interaction with adaptors GGA and PACS-1. J Biol Chem. 2007 Nov 9;282(45):32956-64. PubMed.
- Liang X, Slifer M, Martin ER, Schnetz-Boutaud N, Bartlett J, Anderson B, Züchner S, Gwirtsman H, Gilbert JR, Pericak-Vance MA, Haines JL. Genomic convergence to identify candidate genes for Alzheimer disease on chromosome 10. Hum Mutat. 2009 Mar;30(3):463-71. PubMed.
- Goodarzi MO, Lehman DM, Taylor KD, Guo X, Cui J, Quiñones MJ, Clee SM, Yandell BS, Blangero J, Hsueh WA, Attie AD, Stern MP, Rotter JI. SORCS1: a novel human type 2 diabetes susceptibility gene suggested by the mouse. Diabetes. 2007 Jul;56(7):1922-9. PubMed.
External Citations
Further Reading
Papers
- Small SA, Kent K, Pierce A, Leung C, Kang MS, Okada H, Honig L, Vonsattel JP, Kim TW. Model-guided microarray implicates the retromer complex in Alzheimer's disease. Ann Neurol. 2005 Dec;58(6):909-19. PubMed.
- Rogaeva E, Meng Y, Lee JH, Gu Y, Kawarai T, Zou F, Katayama T, Baldwin CT, Cheng R, Hasegawa H, Chen F, Shibata N, Lunetta KL, Pardossi-Piquard R, Bohm C, Wakutani Y, Cupples LA, Cuenco KT, Green RC, Pinessi L, Rainero I, Sorbi S, Bruni A, Duara R, Friedland RP, Inzelberg R, Hampe W, Bujo H, Song YQ, Andersen OM, Willnow TE, Graff-Radford N, Petersen RC, Dickson D, Der SD, Fraser PE, Schmitt-Ulms G, Younkin S, Mayeux R, Farrer LA, St George-Hyslop P. The neuronal sortilin-related receptor SORL1 is genetically associated with Alzheimer disease. Nat Genet. 2007 Feb;39(2):168-77. PubMed.
- Dodson SE, Gearing M, Lippa CF, Montine TJ, Levey AI, Lah JJ. LR11/SorLA expression is reduced in sporadic Alzheimer disease but not in familial Alzheimer disease. J Neuropathol Exp Neurol. 2006 Sep;65(9):866-72. PubMed.
- Schmidt V, Sporbert A, Rohe M, Reimer T, Rehm A, Andersen OM, Willnow TE. SorLA/LR11 regulates processing of amyloid precursor protein via interaction with adaptors GGA and PACS-1. J Biol Chem. 2007 Nov 9;282(45):32956-64. PubMed.
- Muhammad A, Flores I, Zhang H, Yu R, Staniszewski A, Planel E, Herman M, Ho L, Kreber R, Honig LS, Ganetzky B, Duff K, Arancio O, Small SA. Retromer deficiency observed in Alzheimer's disease causes hippocampal dysfunction, neurodegeneration, and Abeta accumulation. Proc Natl Acad Sci U S A. 2008 May 20;105(20):7327-32. PubMed.
- Liang X, Slifer M, Martin ER, Schnetz-Boutaud N, Bartlett J, Anderson B, Züchner S, Gwirtsman H, Gilbert JR, Pericak-Vance MA, Haines JL. Genomic convergence to identify candidate genes for Alzheimer disease on chromosome 10. Hum Mutat. 2009 Mar;30(3):463-71. PubMed.
Primary Papers
- Lane RF, Raines SM, Steele JW, Ehrlich ME, Lah JA, Small SA, Tanzi RE, Attie AD, Gandy S. Diabetes-associated SorCS1 regulates Alzheimer's amyloid-beta metabolism: evidence for involvement of SorL1 and the retromer complex. J Neurosci. 2010 Sep 29;30(39):13110-5. PubMed.
Annotate
To make an annotation you must Login or Register.

Comments
UCLA/VA
It is intriguing that SorCS1 (see AlzGene) has gender differences in functional effects on Aβ production as well as in the Liang et al., 2009, linkage study. Of course, it makes sense in that it ties into the overall story that genetic differences that increase Aβ production increase risk. It would be nice to see particular genetic variants influencing Aβ production rather than the manipulations of the whole protein level, but that is where we are with SorLA and now with SorCS1.
The issues with both SorLa and now SorCS1, and in fact with nearly every genetic risk factor beyond ApoE, are that most seem tied to Aβ accumulation, the effect size of polymorphisms is low, and specific functional mutations or alleles are not very clear. Modest effect sizes for SNPs in these genes don't mean you won't have potentially important targets for lowering Aβ. However, therapeutic relevance may be limited by issues of specificity with the more basic downstream sorting machinery for proteins like SorCS1. The closer you get to the secretases, the better chance you have for specificity and good therapeutic targets. So I would place SorCS1 in the category of potentially relevant.
That said, over a lifetime, small differences in sorting rates from variants that modestly impact Aβ production rates may have dramatic long term impact. You can make the analogy to compound interest rates, where a quarter point or half point difference in interest seems trivial and doesn't make a significant difference in an 18 month investment portfolio (or clinical trial) but adds up over the decades to really make a difference. My view is that SorLA and SorCS1 and other candidate late-onset AD genes tied to Aβ accumulation are best thought of in the context of prevention. Can we find safe ways to influence them that shift the long-term Aβ balance sheet in our favor?
References:
Liang X, Slifer M, Martin ER, Schnetz-Boutaud N, Bartlett J, Anderson B, Züchner S, Gwirtsman H, Gilbert JR, Pericak-Vance MA, Haines JL. Genomic convergence to identify candidate genes for Alzheimer disease on chromosome 10. Hum Mutat. 2009 Mar;30(3):463-71. PubMed.
�
I love reading these stories. It makes me extremely knowledgeable.
Make a Comment
To make a comment you must login or register.