Miami: Age and Amyloid—What Has ApoE Got to Do With It?
Quick Links
At this stage of Alzheimer's disease research, scientists know that APP or presenilin mutations and the risk gene ApoE4 have two things in common. Both bring down the carrier’s age of disease onset, ApoE4 less drastically than the deterministic mutations. Also, both types of genetic risk push brain amyloid deposition back to younger ages. At the Human Amyloid Imaging Conference, held 12-13 January 2012 in Miami, Florida, several labs presented new data on the connection between ApoE and amyloid deposition in preclinical AD and aging. They are trying to pinpoint when it first deposits and when it might start affecting cognition.
First off, however, a counterpoint to ApoE4. The ApoE2 allele is known to protect against Alzheimer’s, but because it is rare, few studies have been able to look at its mechanism. At HAI, Eisuke Haneda of the Tokyo Metropolitan Institute of Gerontology, Japan, and colleagues reported data from a joint analysis of U.S.-ADNI, the Japanese ADNI, and the Australian Imaging, Biomarker & Lifestyle Flagship Study of Ageing (AIBL). Together, these three studies count at least 24 people with ApoE2 among them. On a poster, Haneda showed that homozygous and heterozygous ApoE2 carriers were much more likely to be amyloid negative in their respective study’s baseline scan than ApoE4 carriers, and even those who did have some amyloid had less of it in the cortex and precuneus (Haneda et al., 2012).
Presenting the first of many studies on ApoE4, Christopher van Dyck of Yale University of Medicine in New Haven, Connecticut, ran PIB scans on cognitively normal volunteers in their fifties and early sixties who had a parent with AD. His study was small—15 people each for the ApoE4/4, 4/3, and 3/3 genotypes. (Like ApoE2, ApoE4 homozygosity is rare, making study participants hard to find.) In this first cross-sectional comparison, PIB uptake was higher in people with the 4/3 genotype than in the 3/3s, and higher still in the 4/4s. The youngest person with significant PIB uptake was a 51-year-old homozygous E4 carrier. In this age group, van Dyck’s group was unable to detect any effect of their amyloid positivity on neuropsychologic performance. That said, most tests used in this study have their greatest dynamic range later, when people are already cognitively impaired, and hence might not have picked up subtle decrements in this age group. Longitudinal studies of this cohort might reveal an association with cognition later on, scientists noted during subsequent discussion (van Dyck et al., 2012).
Two studies presented longitudinal data on cognitively normal cohorts genotyped for ApoE, though these study volunteers are a bit older. Jessica Langbaum of the Banner Alzheimer’s Institute in Phoenix, Arizona, reported two-year PIB-PET data on cognitively normal people in their sixties. This group includes eight ApoE4/4 carriers. Two years after their initial scan (Reiman et al., 2009), they were still cognitively normal, Langbaum said. PIB uptake was again markedly higher in E4 homozygotes and heterozygotes than E4 non-carriers, and it had increased from the baseline scan. In particular, β amyloid accumulated in the prefrontal, lateral, parietal, and precuneus regions of the brain. Langbaum noted that once a person has brain amyloid deposition, it is there to stay. Indeed, multiple scientists doing their own longitudinal studies agreed that, unlike a diagnosis of MCI, where a fraction of patients revert to normal cognition some years later, preclinical amyloid deposition stays and grows in all people repeatedly scanned thus far (Fleisher et al., 2012).
A third study in cognitively normal people offered a breakdown of amyloid deposition by ApoE status. Andrei Vlassenko of Washington University School of Medicine, St. Louis, Missouri, reported changes in between two PIB scans that were, on average, 2.6 years apart. This study included 146 people aged 45 to 86 who were cognitively normal with a CDR of 0 at both time points. Of them, 21 were positive at the first scan and stayed positive at the second scan, whereas 115 were negative at the first and still negative at the second scan. Ten people crossed the threshold from negative to positive between scans. Recently, the scientists started third scans in this cohort. Of 12 people analyzed so far, 11 remain amyloid negative; one person who had previously crossed the threshold demonstrated continuing β amyloid accumulation in a linear fashion, Vlassenko said. In these people, scientists in essence can catch the first glimpses of fibrillar amyloid deposition in a person’s life. The average age of this group was 65; the youngest converter was a 56-year-old man with two copies of ApoE4. Seven of the 10 converters were ApoE4-positive, though it should be noted that this sample is enriched for ApoE4 carriers.
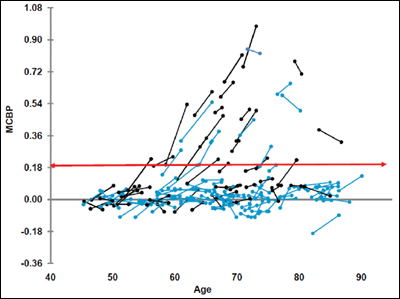
Repeat measurements show brain Aβ levels cross the threshold (red) and increase with age in people with (black) or without (blue) ApoE4. View larger image. Image credit: Vlassenko et al., 2011
With these numbers, the scientists can begin to calculate incidence of conversion. It came out to 3.1 percent for the whole group, and 7 percent for ApoE4 carriers, though these numbers may well change as more people in narrower age ranges have longitudinal scans. Part of these data recently appeared in Annals of Neurology (Vlassenko et al., 2011). "For the first time in the literature, we describe the conversion from no preclinical AD to preclinical AD," said Vlassenko. At HAI, scientists at Avid Pharmaceuticals, the Philadelphia-based company that develops florbetapir, reported a similar 3.5 percent annual conversion rate of people who were amyloid negative at baseline but positive in a subsequent scan.
Where did the amyloid first crop up in these converters? “It’s really quite broad,” Vlassenko said, with highest retention seen in posterior and anterior cingulate, precuneus, lateral and medial frontal cortex. Most people showed an increase in their PIB retention between the first and subsequent scans, which fits with the increase in fibrillar amyloid seen in early MCI (Vlassenko et al., 2012).
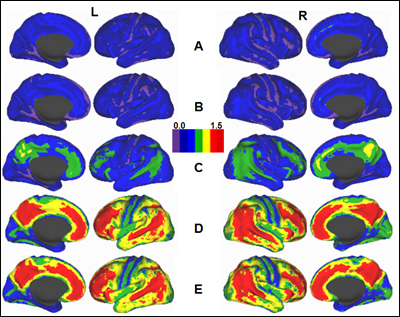
PIB distribution on lateral and medial surfaces of the cortex on the left and right hemispheres of the human brain. A, Healthy adults younger than 50 y; B-D, Cognitively normal adults older than 50 with low (B), moderate (C), and high (D) Aβ deposition; E, Individuals with Alzheimer's dementia. View larger image. Image credit: Vlassenko et al., 2012
The question of when in life amyloid plaques begin to settle in the brain was the subject of a talk by Ozioma Okonkwo at the University of Wisconsin School of Medicine in Madison. Okonkwo analyzed data from 200 cognitively normal people, mostly in their fifties and sixties, who participate in a multimodal imaging substudy of the Wisconsin Registry for Alzheimer’s Prevention, a larger longitudinal study of about 1,500 middle-aged and older adults. PIB scans available so far on 156 of these 200 people show that at baseline, 28 percent of them were amyloid positive. The posterior cingulate, precuneus, and other cortical midline structures were the most susceptible to amyloid aggregation, Okonkwo said. In this sample, although some people younger than 55 years old were amyloid positive, clear-cut elevation in amyloid accumulation appeared to begin at age 55. Here, too, ApoE4 was the strongest predictor of amyloid positivity, with 54 percent of the amyloid-positive participants carrying at least one allele, versus 27 percent of the amyloid-negative participants (Okonkwo et al., 2012). This study also is enriched for ApoE4 relative to the population at large.
Furthermore, Okonkwo noted that fibrillar amyloid aggregation was associated with cortical thinning and hippocampal atrophy. Surprisingly, higher amyloid deposition was also associated with elevated cerebral metabolism and better performance on certain memory tests, perhaps as a reflection of compensatory processes at this cognitively normal stage. MCI studies have previously noted hypermetabolism by FDG-PET in early MCI, versus hypometabolism by late MCI.
Okonkwo noted that the WRAP study focuses on the effect of family history, and, consequently, he looked into what having a parent with AD did to a person’s chances of having brain amyloid in late middle age. Surprisingly, in this initial analysis of a relatively young cohort (mean age was 59), family history did not significantly affect amyloid deposition. On this question of family history, Jacqueline Maye of Massachusetts General Hospital added data into a mysterious new line of research. Some recent studies have observed that a mother’s Alzheimer’s is a more ominous portent than a father’s for an adult child’s prospect of getting the disease, though other studies have not found this. Moreover, some studies have detected a more AD-like imaging pattern in cognitively normal middle-aged people whose mothers had AD. How amyloid PET might enter into this picture is unclear.
Maye looked at this question in 102 cognitively normal or mildly impaired participants in the Harvard Aging Brain Study in whom she was able to determine at what age the parent had become symptomatic with dementia that was likely due to AD. For 32 of them, their mothers had had AD, in 14, the fathers. What did their PIB scans show? This study required controls on many sources of variation, including the child’s age, gender, CDR status, ApoE status, and education. When all this was done, the data still showed that PIB retention was higher in adult children of demented mothers than either children of demented fathers or children without a family history of dementia. Particularly worrisome for those adult children of affected mothers might be that the earlier in life the mother got dementia, the more pronounced was the effect of higher PIB retention in the adult child. This effect held true for sons and daughters, and it is separate from ApoE, Maye said (Maye et al., 2012).
Still more normal aging studies elsewhere have added amyloid imaging to how they assess their cohorts. At HAI, Gerard Bischof at the University of Texas at Dallas teased apart the effects of brain amyloid and white matter hyperintensities in the Dallas Lifespan Brain Study. This is a sample of aging people selected for their robust overall health, i.e., they have no cardiovascular disease, diabetes, or other common diseases of aging. In the 89 people aged 50 and up whom Bischof analyzed, amyloid burden not only increased with age, but each type of brain lesion also appeared to do its independent share of damage to the brain. White matter changes affected reasoning and, perhaps surprisingly, episodic memory, whereas β amyloid as shown by florbetapir hampered working memory, executive function, and processing speed (Bischof et al., 2012).
Studies across continents have been finding a link among ApoE status, age, and brain amyloid with such consistency that some researchers are even entertaining the idea of viewing ApoE and age as a proxy for brain amyloid. This could potentially save costs for secondary prevention trials, noted Michelle Mielke of the Mayo Clinic in Rochester, Minnesota. Mielke reported that in the Mayo Clinic Study of Aging, a population-based normal aging study, 483 people age 70 and older have had PIB-PET scans, and about a third them were positive. Mielke calculated how well other AD risk factors captured in this study might predict PIB positivity as a way of helping secondary prevention trials enrich for brain amyloid without having to go to the expense of screening large numbers of people with PET imaging. Predictably, perhaps, age and ApoE genotype came out on top, suggesting that these two factors can flag the likely presence of brain amyloid (Mielke et al., 2012). Cognitive performance or family history added little in the way of predictive value, Mielke reported.
What about people in their eighties and nineties? In general, scientists poorly understand the role of amyloid in the very old, and this knowledge gap was widely discussed at HAI. The oldest people in Vlassenko’s study, for example, were in their eighties; they appeared to form an exception to the perceived rule of amyloid deposition growing or staying stable over time in that their amyloid retention appeared to dip a bit from one scan to the next. But even among the oldest old, amyloid deposition appears to be bad news. Claudia Kawas of the University of California, Irvine, in a lecture on dementia in the oldest old, showed florbetapir imaging on 13 participants in the longitudinal, population-based 90+ Study. One person who underwent an amyloid PET scan was 99.9 years old, Kawas said. Against her expectations, Kawas found that people who had low amyloid uptake on their scan remained cognitively stable over the 1.5 years of follow-up data available so far, whereas the four participants who had high uptake declined steeply over the course of the next year. “I was shocked by this,” Kawas said. This appears to contradict the idea that amyloid is less related to dementia in the oldest old than in younger people (see, e.g., ARF related news story).
"It's very important that we learn as much as possible about what is going on in the brain before cognitive symptoms arise," said Nordberg. "That will give us a lot of information to really understand the time course of pathological changes." There was wide agreement that larger numbers of people will need to be monitored for at least 10 years with periodic amyloid PET and other risk factor and biomarker assessments before scientists can predict who is going to develop AD and when. In the meantime, there is already broad agreement that cognitively normal or minimally impaired people with amyloid deposition are becoming an important population for early-stage intervention trials.—Gabrielle Strobel.
This is Part 6 of a nine-part series. See also Part 1, Part 2, Part 3, Part 4, Part 5, Part 7, Part 8, Part 9. Download a PDF of the entire series.
References
News Citations
- Oldest Old—The New Face of Dementia?
- News Focus: 2012 Human Amyloid Imaging Conference
- Miami: Amyloid PET in the Clinic: What Are the Issues?
- Miami: Scan and Tell? Amyloid Imaging Confronts Disclosure Dilemma
- Miami: Can the Naked Eye Tell When a Scan Is Positive?
- Miami: When Does Amyloid Deposition Start in Familial Alzheimer’s?
- Miami: Longitudinal Amyloid PET Data Start Converging
- Miami: Diagnosis and Amyloid Scan Can Be at Odds
- Miami: Scientists Angle for Way to Image Tangle
Paper Citations
- Haneda E, Ishii K, Sakata M, Oda K, Toyohara J, Ishiwata K, Senda M, Ito K, Kuwano R, Iwatsubo T. Influence of APOE2 Genotype on Global and Regional Amyloid Deposition. Human Amyloid Imaging Abstract. 2012 Jan 1;
- van Dyck C, Barcelos N, Brück A, Planeta-Wilson B, Benincasa A, MacAvoy M, Gelernter J, Carson R. Amyloid-Beta Burden and Neuropsychological Test Performance in Cognitively Normal First-Degree Relatives at Varying Genetic Risk for Alzheimer's Disease. Human Amyloid Imaging Abstract. 2012 Jan 1;
- Reiman EM, Chen K, Liu X, Bandy D, Yu M, Lee W, Ayutyanont N, Keppler J, Reeder SA, Langbaum JB, Alexander GE, Klunk WE, Mathis CA, Price JC, Aizenstein HJ, Dekosky ST, Caselli RJ. Fibrillar amyloid-beta burden in cognitively normal people at 3 levels of genetic risk for Alzheimer's disease. Proc Natl Acad Sci U S A. 2009 Apr 21;106(16):6820-5. PubMed.
- Fleisher A, Esque J, Chen K, Monarrez C, Liu X, Lee W, Roontiva A, Thiyyagura P, Langbaum J, Bandy D. Tracking Fibrillar Amyloid Accumulation and Estimating Prevention Trial Sample Sizes in Cognitively Normal APOE E4 Homozygotes, Heterozygotes and Non-Carriers. Human Amyloid Imaging Abstract. 2012 Jan 1;
- Vlassenko AG, Mintun MA, Xiong C, Sheline YI, Goate AM, Benzinger TL, Morris JC. Amyloid-beta plaque growth in cognitively normal adults: longitudinal [11C]Pittsburgh compound B data. Ann Neurol. 2011 Nov;70(5):857-61. PubMed.
- Vlassenko A, Blazey T, Su Y, Xiong C, Goate A, Benzinger T, Mintun M, Morris J. Conversion to Preclinical Alzheimer’s Disease in Cognitively Normal Adults: The Characteristics from Longitudinal [11C] PIB PET Study. Human Amyloid Imaging Abstract. 2012 Jan 1;
- Vlassenko AG, Benzinger TL, Morris JC. PET amyloid-beta imaging in preclinical Alzheimer's disease. Biochim Biophys Acta. 2012 Mar;1822(3):370-9. PubMed.
- Okonkwo O, Oh J, Christian B, Xu G, Cleary C, Harding S, Wooten D, Hillmer A, Murali D, Barnhart T. Fibrillar Amyloid-Β Burden in Cognitively Normal Middle-Aged Adults Enrolled in the Wisconsin Registry for Alzheimer’s Prevention. Human Amyloid Imaging Abstract. 2012 Jan 1;
- Maye J, Gidicsin C, Pepin L, Becker JA, Blacker D, Rentz D, Locascio J, Marshall G, Amariglio R, Lorius N. Maternal Dementia Age of Onset in Relation to Amyloid Burden in Non-Demented Offspring. Human Amyloid Imaging Abstract. 2012 Jan 1;
- Bischof G, Rodrigue K, Kennedy K, Devous M, Rieck J, Park D. Beta-Amyloid Deposition and White Matter Hyperintensities Both Contribute To Age-Related Decline in Cognition in Healthy Adults. Human Amyloid Imaging Abstract. 2012 Jan 1;
- Mielke M, Wiste H, Wiegand S, Knopman D, Lowe V, Roberts R, Swenson-Dravis D, Boeve B, Petersen R, Jack C. Predictors of Amyloid Accumulation in a Population-Based Study of Cognitively Normal Elderly Controls. Human Amyloid Imaging Abstract. 2012 Jan 1;
Other Citations
Further Reading
Annotate
To make an annotation you must Login or Register.

Comments
No Available Comments
Make a Comment
To make a comment you must login or register.