HHS Adds Goal of Alzheimer’s Prevention to National Plan
Quick Links
With a new year around the corner, a commitment to a healthier life springs to mind for many, including those in government agencies. Yesterday, U.S. Health and Human Services Secretary Xavier Becerra announced an update to NAPA, the National Plan to Address Alzheimer’s disease. HHS added a sixth goal to the plan, which sets targets for coordinating AD research, care, and treatment development across federal agencies. The new goal focuses on preventing AD by funding prevention research, by encouraging people to change their health behaviors regarding known risk factors such as physical inactivity, unhealthy diet, smoking or drinking, and by better integrating risk reduction strategies for hypertension and diabetes into clinical practice.
“While clinical trials continue to investigate the best therapies to treat and prevent dementia, this new goal will empower individuals, families, and clinicians to work together to make lifestyle changes that could lower their baseline risk for dementia and other age-related diseases,” Cynthia Carlsson, University of Wisconsin, Madison, wrote to Alzforum (full comment below).
Carlsson chairs NAPA’s advisory council, which recommended adding this new goal to the National Plan last July (National Plan to Address Alzheimer's Disease: 2021 Update). The National Plan now comprises six goals, encompassing various aspects of prevention, treatment, and care (see image below).
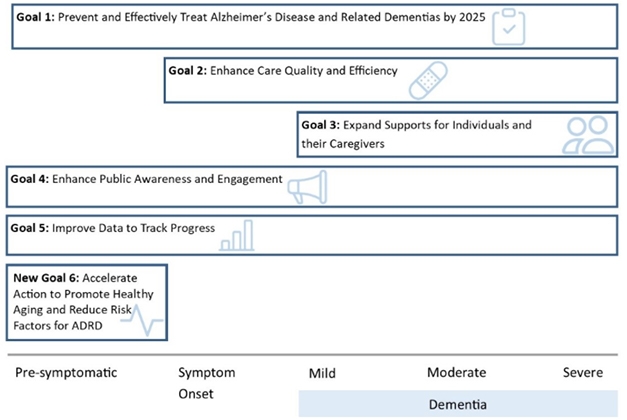
Winning Strategy? The six goals of the National Plan to Address AD. [Courtesy of HHS.]
The addition comes after research and trials have identified modifiable health and welfare factors that increase risk for dementia. Last year, a Lancet Commission concluded that 40 percent of dementia cases could be prevented by tackling 11 such factors (Aug 2020 news).
Under the new goal, the federal government will fund research on risk factors, focusing on how they vary across demographic groups. For example, higher average blood pressure in midlife is tied to faster cognitive decline, with worse outcomes. Uncontrolled high blood pressure in middle-aged black individuals may partly explain disparities in rates of dementia in later life (Levine et al., 2020). Reducing systolic blood pressure over three years cut dementia risk by 19 percent in people over 50 (Jan 2019 news; Aug 2019 news). In a bid to tackle hypertension, the new goal instructs the Food and Drug Administration to establish voluntary sodium content guidelines aiming to lower salt content in processed and prepared foods. Other research areas singled out by the goal include traumatic brain injury and COVID-19.
HHS also aims to improve access to devices that could help reduce dementia risk, such as hearing aids. Hearing loss in midlife increases risk for dementia. In this spirit, last October the FDA proposed a rule to let people skip the medical exam and audiologist fitting and purchase hearing aids directly in-store or online (FDA press release).
Additionally, HHS hopes to strengthen the infrastructure needed to educate the public, caregivers, and health care providers on reducing risk, including from chronic conditions associated with dementia. The department will fund public health campaigns and expand the delivery of health programs to older adults in underserved areas. The Centers for Disease Control will convene a national summit conference next year to establish public health priorities to reduce dementia risk.—Chelsea Weidman Burke
References
News Citations
- Lancet Commission’s Dementia Hit List Adds Alcohol, Pollution, TBI
- SPRINT MIND Data Published, Follow-Up Extended
- Blood Pressure: How Low to Prevent Dementia—and When?
Paper Citations
- Levine DA, Gross AL, Briceño EM, Tilton N, Kabeto MU, Hingtgen SM, Giordani BJ, Sussman JB, Hayward RA, Burke JF, Elkind MS, Manly JJ, Moran AE, Kulick ER, Gottesman RF, Walker KA, Yano Y, Gaskin DJ, Sidney S, Yaffe K, Sacco RL, Wright CB, Roger VL, Allen NB, Galecki AT. Association Between Blood Pressure and Later-Life Cognition Among Black and White Individuals. JAMA Neurol. 2020 Jul 1;77(7):810-819. PubMed.
External Citations
Further Reading
News
Annotate
To make an annotation you must Login or Register.

Comments
University of Wisconsin School of Medicine and Public Health
The National Plan to Address Alzheimer’s Disease has played an important role in coordinating efforts in research, clinical care, and support services among many stakeholders, including federal and non-federal agencies, persons living with dementia, their care partners, and many other advocates.
The new goal focusing on healthy aging and risk reduction of Alzheimer’s and related dementias will accelerate research on the impact of treating modifiable risk factors, such as high blood pressure, depression, and sleep disorders, on cognitive decline and dementia.
While clinical trials continue to investigate the best therapies to treat and prevent dementia, this new goal will empower individuals, families, and clinicians to work together to make lifestyle changes that could lower their baseline risk for dementia and other age-related diseases. This new risk-reduction goal will also foster collaboration between research and public health initiatives aimed at improving health equity in diverse communities.
Make a Comment
To make a comment you must login or register.